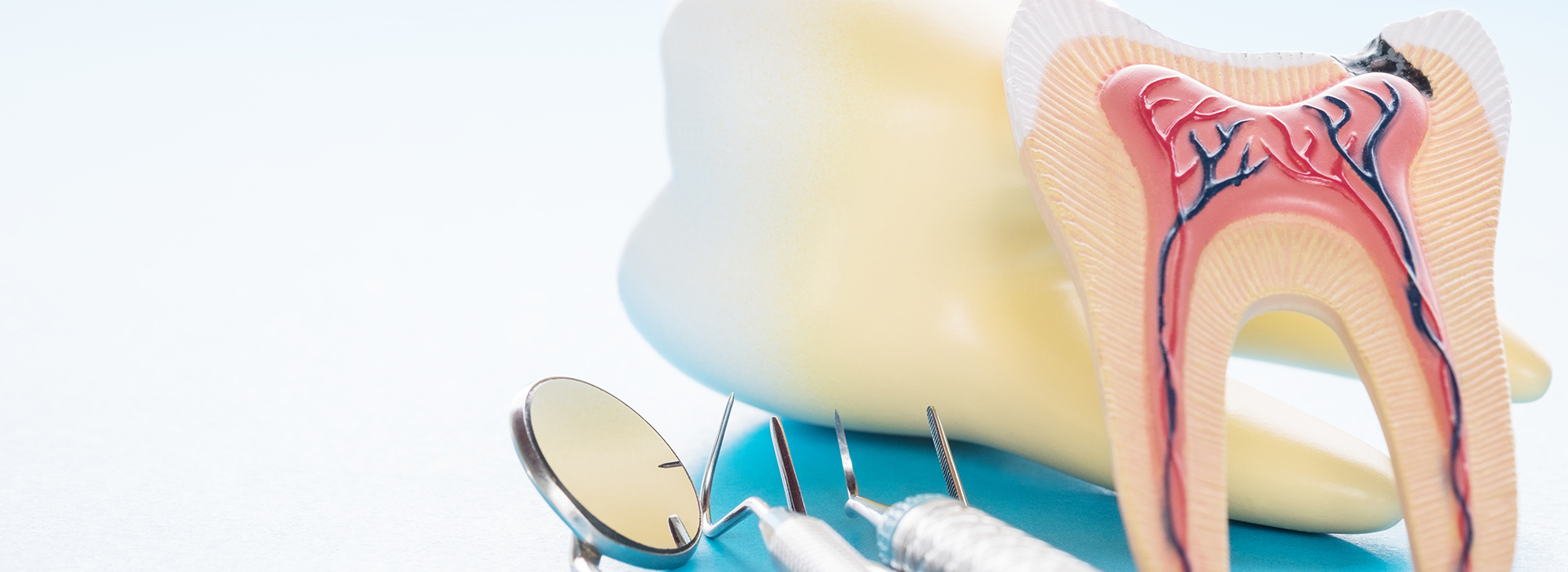
Being told a tooth needs a root canal can feel worrying, but modern care has made the procedure routine, predictable, and focused on your comfort. Root canal therapy is designed to remove damaged tissue inside a tooth, stop infection, and restore function so you can keep your natural tooth rather than losing it to extraction.
At Ramsi Dental, we combine careful diagnosis with contemporary techniques to deliver precise, comfortable root canal care. Our goal is to help you understand the reasons for treatment, what the procedure involves, and how to protect your smile afterward.
Choosing to preserve a natural tooth whenever possible has benefits beyond appearance. A natural tooth maintains the alignment and function of your bite, supports surrounding teeth, and preserves the underlying jawbone. When a root canal succeeds, it often restores long-term stability and comfort that a replacement tooth may struggle to match.
Root canal treatment removes the inflamed or infected pulp inside a tooth and seals the canals to prevent recontamination. With appropriate restoration after treatment — most commonly a crown — the treated tooth can withstand normal chewing forces and remain a reliable part of your mouth for years to come.
Advances in materials and instrumentation have improved outcomes and predictability. While no dental procedure guarantees perfection, conservative endodontic care is usually the most reliable option to retain a tooth that otherwise might be lost to extraction and replacement.

The center of every tooth contains soft tissue called the dental pulp: nerves, blood vessels, and connective tissue that guide development and report sensations. When that tissue becomes infected or irreversibly damaged — from deep decay, a crack, or a traumatic blow — it can cause persistent pain, swelling, or eventually spread infection beyond the tooth root.
Symptoms that often point to pulpal damage include lingering sensitivity to hot or cold, pain when biting, discoloration of a single tooth, gum swelling, or a pimple-like drain on the gum. Sometimes, however, a tooth may be largely symptom-free and show signs of trouble only on X-rays; this is why regular exams and imaging are important for early detection.
When a tooth’s pulp cannot recover, root canal therapy becomes the treatment of choice to eliminate infection and preserve the tooth structure. If the root canal is completed and the tooth is properly restored, the tooth can remain functional without the pain or risks associated with infection.
Although not every toothache indicates a need for root canal therapy, watch for these common warning signs that merit prompt evaluation:
Pain that lingers or intensifies, especially when it disturbs sleep or daily activities, can signal significant inflammation or infection within a tooth. Early assessment helps determine whether root canal treatment is needed to stop the process.
Sensitivity that lasts long after exposure to hot or cold items suggests the nerve is involved. While occasional twinges are common, prolonged discomfort points to more advanced pulp irritation.
Pain when biting down or pressure on a particular tooth often accompanies pulpal problems or a developing abscess. This symptom can indicate that inner tissues are compromised and require attention.
A tooth that becomes darker than surrounding teeth may have lost its internal vitality following trauma or longstanding infection. Discoloration is often a visual clue that deeper problems exist beneath the enamel.
Structural damage from injury or biting on hard objects can expose or inflame the pulp. Even if the damage seems minor, the internal tissues may be affected and a root canal could be necessary to save the tooth.
Gum swelling or a localized bump is a sign the infection has reached surrounding tissues. Timely treatment reduces the chance of more extensive problems and helps preserve oral health.
In some cases, infection around the root can affect the bone that supports the tooth, making it feel loose. Treating the source of infection can allow the tissues to heal and restore stability.
Delaying care for a troubled tooth increases the risk of complications. An infection left unchecked can extend to surrounding bone or soft tissues and make eventual treatment more complex. Early diagnosis — often including clinical testing and radiographs — allows for simpler, more predictable treatment.
Not every problematic tooth causes obvious pain at first. Routine exams and X-rays sometimes reveal hidden issues such as bone changes near a root or internal damage that has not yet produced strong symptoms. Identifying these signs early gives you more treatment options and a better chance of preserving the tooth.
When a clinician recommends root canal therapy, it is usually because that approach offers the best balance of conserving tooth structure while resolving infection. Acting promptly reduces the likelihood of emergency situations and supports a smoother recovery.
Root canal procedures today are performed with attention to comfort and precision. The area is numbed with local anesthesia so the treatment is pain-free, and magnification and specialized instruments help the clinician access, clean, and shape the canals carefully.
Some cases are completed in a single visit, while others require multiple appointments depending on the tooth’s anatomy or the presence of active infection. During the appointment, the dentist removes the diseased pulp, disinfects the canal system, and seals the canals with a biocompatible material to prevent reinfection.
For patients who experience dental anxiety or need greater relaxation, sedation options may be discussed to make the visit more comfortable. After the root canal itself, a restorative plan — commonly a crown — will be recommended to protect the tooth and restore full function.
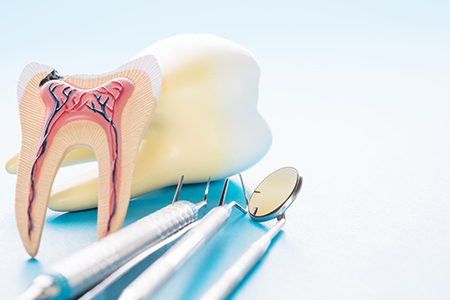
After treatment, it is normal to experience mild soreness for a few days as tissues heal. Over-the-counter pain relievers usually manage post-treatment discomfort, and your clinician will provide tailored instructions for care and any medications that may be needed.
A treated tooth may initially receive a temporary filling; it’s important to complete the recommended restoration, such as a crown, to reinforce the tooth and reduce the risk of fracture. Until that permanent restoration is placed, avoid heavy chewing or sticky foods on the treated side.
Good oral hygiene and regular dental visits help ensure the long-term success of root canal therapy. With appropriate care, many root canal–treated teeth remain functional for decades.
At our practice, we take time to explain each step of treatment and what you can expect during recovery. If you notice persistent symptoms after treatment — increased pain, swelling, or other concerns — contact us for evaluation.
In summary, root canal therapy is a reliable way to relieve pain, stop infection, and save natural teeth when the inner tissues are damaged. If you have symptoms that align with the warning signs described here or have questions about maintaining a treated tooth, please contact us for more information.

A root canal is a treatment that removes infected or damaged pulp from inside a tooth to eliminate pain and stop the spread of infection. The clinician accesses the tooth, cleans and shapes the canal system using specialized instruments, and disinfects the space to remove bacteria and debris. The canal is then filled with a biocompatible material and sealed to prevent recontamination.
Local anesthesia keeps the procedure comfortable, and magnification or advanced instrumentation improves precision and outcomes. Depending on the tooth and clinical situation, a temporary restoration may be placed before a final crown or other restoration is completed. The goal is to preserve the natural tooth and restore normal function while reducing the risk of future infection.
Common signs that suggest pulp damage include persistent toothache, lingering sensitivity to hot or cold, pain when biting, swelling, or a pus-filled bump on the gum near the tooth. A single tooth that becomes discolored after trauma can also indicate loss of internal vitality. Because some teeth show little or no symptoms, diagnostic tools such as clinical testing and X-rays are important for accurate assessment.
A clinician evaluates symptoms, performs tests, and reviews radiographs to determine whether the pulp can recover or requires treatment. Timely diagnosis increases the chances of saving the tooth with root canal therapy and avoids complications that can arise from untreated infection. If you notice any of the warning signs, prompt evaluation is recommended to identify the best course of care.
Modern root canal treatment is performed with local anesthesia and techniques that make the procedure no more uncomfortable than a routine filling for most patients. Many people actually experience relief from the severe tooth pain that prompted treatment once the infection is removed. Sedation options can be offered for patients with anxiety to improve comfort and reduce stress.
It is normal to feel mild soreness or tenderness for a few days after the procedure as surrounding tissues heal, and over-the-counter pain relievers typically control this discomfort. Significant or increasing pain, swelling, or other concerning symptoms are uncommon but should prompt a follow-up appointment. Your clinician will provide specific aftercare instructions and guidance on when to contact the office.
Appointment length and the number of visits depend on the tooth's anatomy and whether active infection is present; many uncomplicated cases are completed in a single visit lasting roughly 60 to 90 minutes, while molars or infected teeth may require additional time. Complex canal systems or the need for antimicrobial dressing between visits can extend treatment to multiple appointments to ensure thorough disinfection. The dentist will explain the anticipated plan after diagnosis so you know what to expect.
If more than one visit is needed, a temporary filling is placed to protect the tooth between appointments and reduce sensitivity. After root canal treatment is finished, a final restoration such as a crown is typically scheduled to protect the tooth and restore strength. Completing the restorative step in a timely manner helps ensure long-term success of the treatment.
Recovery usually involves mild tenderness for a few days as the surrounding tissues heal and inflammation subsides. Patients are advised to avoid heavy chewing on the treated tooth until the final restoration is placed and to maintain gentle oral hygiene around the area. Most post-treatment discomfort is manageable with over-the-counter medications and short-term care instructions from the clinician.
If pain increases, swelling develops, or you notice persistent drainage or fever, contact the dental team for evaluation because these signs may indicate a complication. Follow-up visits and radiographs help the clinician confirm healing and the integrity of the restoration. Good home care and routine dental checkups support the long-term health of the treated tooth.
Because root canal treatment removes internal tissue and often requires access through the chewing surface, a protective restoration is commonly recommended to restore strength and prevent fracture. Molars and premolars frequently receive crowns to redistribute biting forces and seal the tooth against recontamination. The type of restoration depends on how much natural tooth structure remains and the tooth's function in the mouth.
At Ramsi Dental, clinicians plan the restorative phase as part of the overall treatment so the tooth receives appropriate protection once healing begins. Timely placement of the permanent restoration reduces the risk of future problems and supports the long-term success of the root canal. Regular maintenance and avoiding hard or sticky foods on the treated tooth help preserve the restoration and underlying tooth structure.
The primary alternatives to root canal therapy are extracting the affected tooth and replacing it with a dental implant, bridge, or removable partial denture. Each option has clinical trade-offs related to preserving natural tooth structure, bone health, and long-term function. The best choice depends on the tooth's restorability, the extent of infection, overall oral health, and the patient's preferences.
A dentist will review these factors and discuss the pros and cons of conserving the tooth versus replacement to help you make an informed decision. When feasible, preserving the natural tooth is often preferred because it maintains bite alignment and supports surrounding teeth. If extraction is chosen, the clinician will explain replacement options and follow-up care to maintain oral health.
Root canal therapy is generally predictable, but risks include persistent infection, missed canals, root fracture, or the need for retreatment or apical surgery in rare cases. Instrument breakage or incomplete sealing of all canal spaces can compromise outcomes and may require additional procedures. The incidence of serious complications is lowered by thorough diagnosis, modern instruments, and careful technique.
Patients can reduce risk by following pre- and post-treatment instructions, completing the recommended final restoration, and attending follow-up visits for monitoring. If symptoms recur or new concerns arise, prompt evaluation allows the clinician to address problems before they become more complex. Good communication between patient and provider supports timely management of any complications.
Although many root canal–treated teeth function for decades, failure can occur from new decay, structural fracture, or persistent infection in a previously untreated canal. Symptoms of failure include recurring pain, swelling, or a draining sinus tract near the tooth, and radiographs help identify the underlying cause. The treatment plan for a failed root canal may vary depending on the reason for failure and the condition of the remaining tooth structure.
Retreatment of the canal system, endodontic surgery (apicoectomy), or extraction followed by replacement are potential options that a clinician will consider and discuss. Decision-making balances the likelihood of success, the tooth's strategic value in the mouth, and the long-term prognosis. Early assessment and intervention improve the chances of saving the tooth or planning an appropriate replacement strategy.
To promote comfort and predictable results, the practice uses careful diagnosis, digital imaging, local anesthesia, magnification, and contemporary instruments during root canal treatment. Sedation options are available for patients who need extra relaxation, and protocols for infection control and aseptic technique reduce risks during the procedure. Clinicians tailor each treatment plan to the tooth's anatomy and the patient's medical history to support optimal healing.
At Ramsi Dental, we emphasize clear communication, step-by-step explanations, and coordination of the restorative phase so the treated tooth receives the protection it needs after endodontic therapy. Follow-up appointments and periodic radiographs allow the team to monitor healing and intervene if issues arise. Patient education about home care and regular dental visits further contributes to long-term success and comfort.

We’d love to hear from you! Whether you have questions about our services, want to schedule an appointment, need guidance on your dental care, or simply want to learn more about how we can help you achieve a healthy, confident smile, our friendly and knowledgeable team is here to assist you.
Visit us at Ramsi Dental or reach out by phone or through our online form. We’re committed to making your experience easy, welcoming, and stress-free, and we’ll respond promptly to ensure you get the care you need.