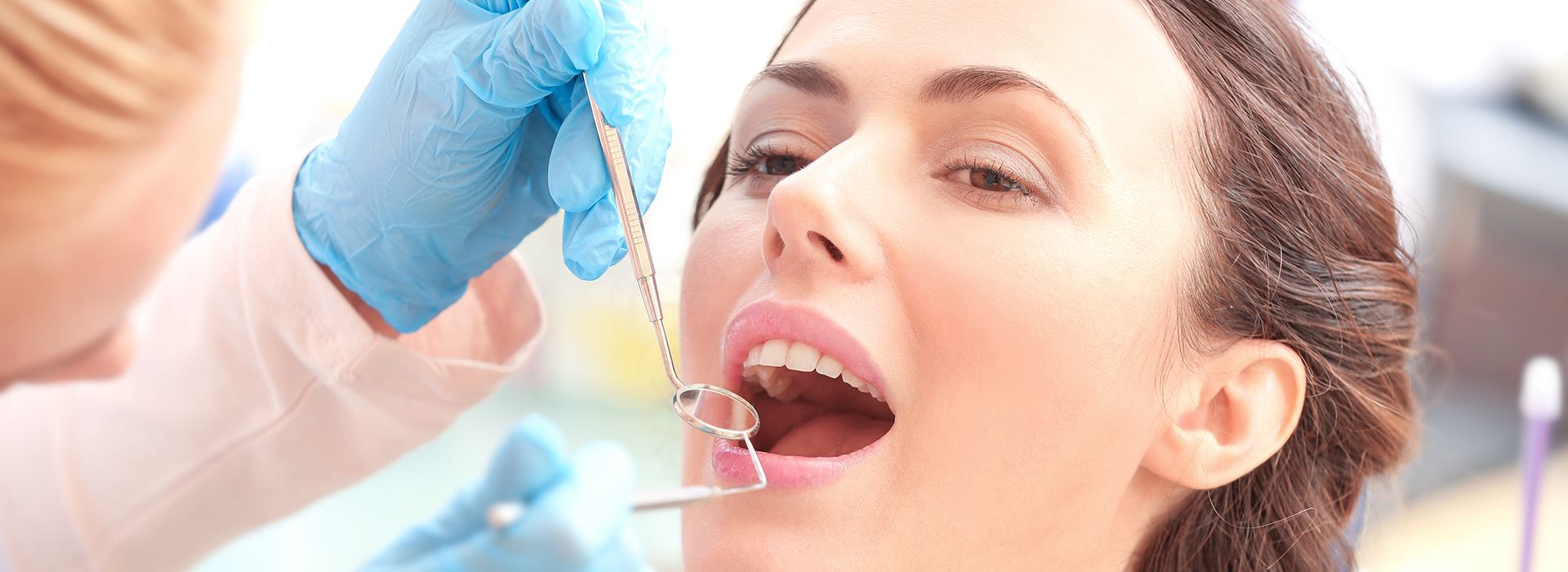
Gum disease is the leading cause of adult tooth loss, yet it's also one of the most preventable conditions affecting oral health. Studies show that periodontal problems are common among adults, and early attention makes a major difference in outcomes. At the office of Ramsi Dental, we focus on clear diagnosis, practical prevention, and personalized treatment plans to help patients protect the tissues that keep their smiles stable and functional.
Periodontal disease refers to a group of inflammatory conditions that target the periodontium — the gums, the connective tissues that anchor teeth, and the underlying jawbone. It begins when bacterial biofilm (plaque) builds up at and below the gumline. Over time, toxins produced by these bacteria trigger inflammation, damaging the soft tissues and, in advanced cases, eroding the bone that supports teeth.
Because early stages of gum disease often produce minimal pain, many people don't realize anything is wrong until signs become more obvious. That’s why routine dental exams and cleanings are essential: they let clinicians identify subtle pockets of inflammation, measure tissue health, and intervene before irreversible changes occur.
Prevention centers on disrupting the bacteria that drive the disease process. Effective daily hygiene, paired with periodic professional care, reduces plaque accumulation and helps tissue heal. When treatment begins early, the inflammatory response can usually be controlled and long-term damage avoided.
Common warning signs that warrant prompt evaluation include:
Gums that appear red, swollen, or tender to the touch
Bleeding during brushing, flossing, or spontaneously while chewing
Gum recession exposing more of the tooth or its root surface
Increased sensitivity to hot, cold, or sweet stimuli
Persistent bad breath or an unpleasant taste in the mouth
Teeth that feel loose, shift position, or create new gaps
Changes in the way dentures or partials fit over time
Discharge or pus around the gumline or between teeth
Discomfort when biting or chewing

Healthy gums do more than preserve your smile; they contribute to overall well‑being. Inflammation that originates in the mouth can influence systemic health, and research continues to explore links between periodontal inflammation and conditions such as cardiovascular disease, diabetes control, and respiratory health. Reducing oral inflammation is therefore a worthwhile part of maintaining general health.
Good preventive habits — including consistent brushing and flossing, avoiding tobacco, and attending scheduled professional cleanings — not only protect against tooth loss but also help lower the burden of chronic inflammation. Regular monitoring allows clinicians to detect subtle changes early and recommend targeted interventions.
Our approach emphasizes measurable goals: reducing pocket depths, improving tissue tone and color, and stabilizing any early bone loss. When patients and their dental team work together, the risk of progressive disease falls considerably.
Gingivitis is the initial, reversible stage of gum disease. It presents primarily as redness, swelling, and bleeding of the gum tissue without permanent loss of bone or connective tissue. Because gingivitis is still a superficial inflammatory response, timely action can typically restore healthy gums.
A focused regimen of professional cleaning and renewed home care — often including more attentive brushing, daily interdental cleaning, and possibly adjunctive antimicrobial rinses as recommended by a clinician — can resolve inflammation. Follow-up appointments are important to confirm that the tissues have recovered and to educate patients about long-term maintenance.
Left unchecked, gingivitis may progress to a deeper infection. That progression is not inevitable, however; with early recognition and consistent care, most people return to healthy periodontal conditions without surgical intervention.

Periodontitis occurs when inflammation spreads beneath the gumline and begins to damage the fibers and bone that stabilize teeth. As pockets form between the tooth and surrounding tissue, bacteria and their byproducts thrive in areas that are difficult to clean with routine hygiene alone. Over time this leads to progressive attachment loss and, in some cases, tooth mobility or loss.
The goals of treatment at this stage are to arrest the infection, reduce pocket depth, and regenerate or preserve as much supporting tissue as possible. A thorough clinical exam — including pocket measurements and radiographs when indicated — informs a tailored treatment plan designed to address the specific pattern and severity of disease.
Modern periodontal care combines mechanical removal of bacterial deposits with adjunctive therapies as needed. With appropriate intervention and a strong maintenance program, many patients can stabilize their condition and retain natural teeth for many years.
Treatment begins with a detailed assessment of your periodontal status and overall health factors that influence healing. Because each case is unique, care plans are individualized to reflect pocket depth, bone levels, medical history, and patient goals. We emphasize methods that balance effectiveness with minimal invasiveness whenever possible.
Non-surgical therapies are typically the first line of treatment. These efforts focus on thoroughly removing plaque and hardened deposits from root surfaces so that inflamed tissues can heal. When necessary, adjunctive antimicrobial measures can help control bacterial strains that contribute to persistent inflammation.
When deeper damage is present, surgical options may be required to clean infected tissue, reduce pocket depths, or rebuild lost structures. Wherever surgery is indicated, the objective is to restore a healthier environment for the gums and bone and to make ongoing home care more effective.
After assessment, clinicians will recommend the approaches most likely to achieve long-term stability. Treatment often proceeds in stages: initial non-surgical care to control infection, reassessment, and then surgical or regenerative steps if improvement is incomplete. Patient engagement and consistent maintenance visits are essential components of success.
We work with patients to set realistic expectations, explain the benefits and limitations of each option, and outline the maintenance schedule needed to protect results. Education about effective daily care and risk factor modification — such as smoking cessation — is an important part of every program.
Ultimately, the goal is to stop disease progression, preserve natural teeth when possible, and restore a healthier environment in the mouth that supports long-term wellness.
When disease is detected early or tissue response is favorable, non-surgical options are often sufficient. Scaling and root planing — careful removal of plaque and calculus from root surfaces followed by smoothing of the roots — helps eliminate the bacterial reservoirs that sustain inflammation. These procedures are typically performed under local anesthesia for comfort.
Adjunctive measures, such as locally delivered antimicrobials placed below the gumline or short courses of systemic medication when clinically indicated, can support healing. The emphasis is on restoring a clean root surface and reducing pocket depths so that daily hygiene becomes effective again.
With diligent home care and a personalized maintenance schedule, many patients achieve stable periodontal health without needing surgery.
When periodontal pockets are deep (generally beyond what non-surgical therapy can access) or when there has been significant loss of attachment and bone, surgical treatment may be recommended. Procedures such as flap surgery allow the clinician to lift the gum tissue, thoroughly clean the roots and bone, and reshape or graft tissues to reestablish healthier contours.
Regenerative techniques — including bone grafting and the use of biologic materials that encourage tissue regrowth — aim to recover lost supporting structures when feasible. These interventions can improve function, enhance esthetics, and create a more maintainable environment for long-term care.
Contemporary options also include the selective use of laser therapy for specific indications, which can complement conventional surgery in reducing pocket depths and managing inflamed tissue when appropriate.
At the office of Ramsi Dental, our focus is on evidence-based care, clear communication, and durable results. If you have noticed any signs of gum disease or would like to learn more about prevention and treatment options, please contact us for more information.

Periodontal disease is an umbrella term for inflammatory conditions that affect the gums, the connective tissues that anchor teeth, and the supporting jawbone. It begins with bacterial biofilm accumulation at and below the gumline and can range from reversible gingivitis to destructive periodontitis if left uncontrolled. Early stages primarily involve soft tissue inflammation, while advanced stages produce attachment loss and bone erosion that threaten tooth stability.
Recognizing the stage of disease is important because it guides treatment choices and prognosis. Gingivitis is typically reversible with professional cleaning and improved home care, whereas periodontitis often requires more intensive mechanical therapy and ongoing maintenance. With appropriate intervention most patients can stabilize their condition and preserve natural teeth for the long term.
The primary driver of periodontal disease is persistent bacterial biofilm, commonly called plaque, that accumulates around teeth and in periodontal pockets. Bacterial toxins and the body’s inflammatory response to those microbes damage soft tissues and, over time, the supporting bone. The process is dynamic and influenced by how effectively plaque is removed through daily hygiene and professional care.
Several risk factors increase the likelihood or severity of disease, including tobacco use, poorly controlled diabetes, certain medications, genetic predisposition, and chronic stress. Systemic health conditions and lifestyle factors can alter the host response and make periodontal breakdown more likely, so comprehensive care considers both oral and overall health contributors.
Early gum disease often produces subtle signs such as redness, swelling, and bleeding during brushing or flossing that patients may overlook. As inflammation progresses, symptoms can include persistent bad breath, gum recession that exposes root surfaces, increased tooth sensitivity, and the formation of deeper pockets between teeth and gums. In advanced cases people may notice tooth mobility, changes in bite, or discharge from around the gumline.
Because discomfort is not always present, routine dental examinations and periodontal probing are essential to detect disease before significant damage occurs. Monitoring pocket depths, tissue tone, and radiographic bone levels allows clinicians to identify active disease and intervene promptly. Prompt evaluation is recommended whenever warning signs are observed so treatment can begin while outcomes are most favorable.
Diagnosis begins with a thorough clinical examination that includes pocket depth measurements, assessment of gum recession, checking for bleeding on probing, and evaluation of tooth mobility. Radiographs are used when indicated to assess bone levels and the pattern of bone loss, which helps distinguish localized from generalized disease. A careful medical and dental history is also important to identify systemic factors or medications that may affect periodontal health.
At Ramsi Dental clinicians integrate clinical findings with diagnostic imaging to create an individualized treatment plan. Reassessment after initial therapy confirms the tissue response and determines whether additional non-surgical or surgical steps are necessary. This staged approach ensures care is tailored to disease severity and the patient’s overall health status.
The first line of periodontal therapy is typically non-surgical and focuses on thorough mechanical removal of plaque and calculus from root surfaces through scaling and root planing. These procedures are performed with hand instruments and ultrasonic devices, often under local anesthesia for patient comfort, to eliminate bacterial reservoirs and allow inflamed tissues to heal. Adjunctive measures such as locally delivered antimicrobials or short courses of systemic medication may be recommended in select cases to address specific microbial concerns.
After non-surgical therapy patients enter a period of reassessment and maintenance to monitor healing and ensure pocket reduction. Effective home care and a personalized supportive periodontal therapy schedule are essential to preserve gains achieved by treatment. Many patients achieve long-term stability with this combination of professional care and diligent self-care.
Surgery is considered when non-surgical therapy does not sufficiently reduce deep pockets or when there is significant loss of attachment and bone that cannot be accessed or corrected otherwise. Common surgical approaches include flap procedures to expose and clean root surfaces, osseous contouring to reshape bone, and regenerative techniques such as bone grafting or the use of biologic materials to encourage tissue regrowth. The goal of surgery is to create a healthier, maintainable environment and, when possible, to restore lost supporting structures.
Indications for surgery are individualized and based on pocket depth, the pattern of bone loss, tooth prognosis, and patient-specific factors like systemic health and ability to maintain hygiene. Clinicians discuss the expected benefits, risks, and postoperative care so patients can make informed decisions. When indicated, surgery is integrated into a comprehensive plan that includes ongoing maintenance to protect results.
Periodontal inflammation contributes to the body’s overall inflammatory burden and has been associated with a range of systemic conditions in observational studies, including cardiovascular disease, difficulties with glycemic control in diabetes, and adverse respiratory events. While associations do not prove direct causation, reducing chronic oral inflammation is a sensible component of comprehensive health management. Controlling periodontal disease can help lower local and systemic inflammatory mediators and may support better general health outcomes.
Clinicians coordinate care with patients’ medical providers when systemic conditions may influence periodontal treatment or healing. Addressing modifiable risk factors such as smoking and uncontrolled blood sugar is an important part of reducing periodontal risk and improving treatment response. Open communication between dental and medical teams helps ensure safe, effective care for patients with complex health needs.
Prevention centers on disrupting the bacterial biofilm that drives periodontal inflammation through consistent daily hygiene and regular professional care. Brushing twice daily with a fluoride toothpaste, daily interdental cleaning with floss or interdental brushes, and periodic professional cleanings reduce plaque accumulation and help maintain healthy tissues. Lifestyle measures such as avoiding tobacco and keeping systemic conditions like diabetes well controlled further lower risk.
Regular periodontal evaluations allow clinicians to detect early changes and adjust care before irreversible damage occurs. Personalized maintenance intervals and patient education on effective home care techniques are critical to long-term success. When patients follow recommended prevention and maintenance protocols, the likelihood of disease progression drops substantially.
Recovery depends on the type and extent of therapy but commonly involves a period of reduced inflammation, soft tissue healing, and gradual improvement in pocket depths over weeks to months. Patients may experience mild discomfort, swelling, or sensitivity that is managed with short-term analgesics and careful home care as instructed by the clinician. Adhering to postoperative instructions, including temporary modifications to brushing and eating, supports optimal healing.
Long-term maintenance is essential to preserve treatment results and typically involves regular supportive periodontal therapy visits to monitor tissue health and remove any recurrent deposits. Ramsi Dental emphasizes ongoing communication, individualized recall intervals, and reinforcement of effective home care to protect periodontal stability. Consistent follow-up and risk factor management are the foundations of durable outcomes.
Frequency of follow-up depends on disease severity, treatment response, and individual risk factors; there is no single interval that fits every patient. For people with a history of periodontitis, supportive periodontal therapy every three months is commonly recommended to control bacterial repopulation and monitor tissue health, while patients with minimal risk may be seen at longer intervals determined by their clinician. The recall schedule is adjusted based on pocket depths, bleeding on probing, and overall stability.
During maintenance visits clinicians reassess clinical measurements, perform professional cleaning below the gumline when needed, and reinforce home care techniques to prevent recurrence. A collaborative approach between patient and clinician ensures that maintenance intervals remain appropriate as health status and risk factors change. Early detection of recurrent inflammation allows prompt intervention and better long-term preservation of natural teeth.

We’d love to hear from you! Whether you have questions about our services, want to schedule an appointment, need guidance on your dental care, or simply want to learn more about how we can help you achieve a healthy, confident smile, our friendly and knowledgeable team is here to assist you.
Visit us at Ramsi Dental or reach out by phone or through our online form. We’re committed to making your experience easy, welcoming, and stress-free, and we’ll respond promptly to ensure you get the care you need.