
At the office of Ramsi Dental, we approach every extraction with the same priorities: safety, clear communication, and patient comfort. Before any procedure begins, our team reviews your medical and dental histories, asks about current medications, and discusses any conditions that might affect treatment. This pre-procedure conversation allows us to tailor care to your needs and reduce surprises on the day of the appointment.
We know extractions can feel intimidating, so we take time to explain the process in straightforward terms. You’ll learn why the extraction is recommended, what type of removal is anticipated, and the steps we’ll take to manage pain and swelling. Understanding the plan can ease anxiety and help you feel more in control of your care.
Where appropriate, we may recommend diagnostic imaging so the team can see the tooth and the surrounding bone clearly. Digital radiographs are a common and effective tool for mapping root shape, assessing nearby structures, and choosing the safest approach. If there are any special considerations — for example, medication adjustments or a need for medical clearance — we’ll review those in advance.
Primary (baby) teeth that won’t fall out on their own
Sometimes a primary tooth remains secure even as the adult tooth beneath it begins to form. When a baby tooth fails to loosen because its roots haven’t resorbed or it has fused to the jawbone, it can block proper eruption and affect alignment. Removing a retained primary tooth can help the permanent tooth emerge in the right position and avoid future orthodontic complications.
Permanently damaged teeth that cannot be restored
Decay that progresses unchecked can undermine a tooth’s structure and reach the nerve, leaving it beyond repair. When a tooth has lost too much healthy material or the root is compromised, extraction becomes the safest option to stop infection and protect neighboring teeth and tissues. Our goal is always preservation first, but extractions are sometimes the most responsible course of action.
Teeth fractured or broken below the gum line
Severe fractures that extend into the root or are not restorable can leave little choice but removal. Different types of breaks require different responses, and when the remaining tooth is unstable or risks causing further problems, extraction prevents pain and additional complications for surrounding teeth and gums.
Advanced periodontal disease affecting tooth support
When gum disease progresses to the point that bone and soft tissues no longer support a tooth, loosening and infection can occur. In advanced cases, extraction may be necessary to preserve overall oral health and stop the spread of infection. Removing severely compromised teeth also makes it easier to restore gum health and plan for replacement solutions when appropriate.
Problematic wisdom teeth
Third molars often lack sufficient space to erupt properly and can become impacted, angled, or decayed. These conditions can cause pressure, infection, or damage to adjacent teeth. For many young adults, early removal of troublesome wisdom teeth prevents future pain and preserves jaw alignment; for others, monitoring and selective extraction are the best choices.
Extractions as part of orthodontic planning
When the jaw doesn’t have room for all permanent teeth, removing one or more teeth can be part of a broader orthodontic strategy to create space, improve alignment, and establish a functional bite. These decisions are made in collaboration with your orthodontic team to achieve an efficient and stable result.
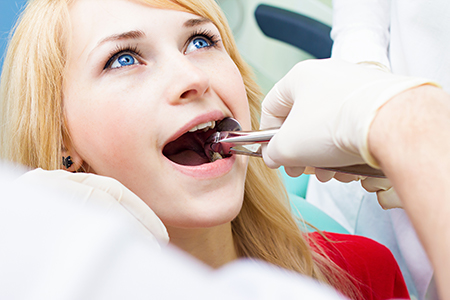
To make a removal as predictable and comfortable as possible, we categorize extractions based on what we see during the exam and on radiographs. Simple extractions involve teeth that are fully visible in the mouth and have straightforward root anatomy. Surgical extractions are reserved for teeth that are broken, impacted, or have unusual root shapes that require a more controlled approach.
For both types, we begin by numbing the area with a local anesthetic and verifying that you’re comfortable. When needed, we can discuss additional comfort measures such as oral sedation to help relaxed patients tolerate the procedure with less stress. Everything we do is aimed at minimizing discomfort and reducing the risk of complications.
During a simple extraction the dentist will gently loosen the tooth and remove it using specialized instruments. Surgical extractions may require a small incision in the gum and selective removal of a bit of bone to access the tooth safely. If a surgical extraction is beyond the scope of in-office treatment, we’ll coordinate a referral to an oral and maxillofacial surgeon and explain what to expect.
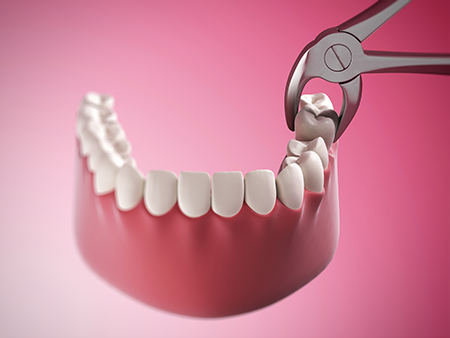
A simple extraction is typically quick and predictable when the crown is intact and the roots are straightforward. After effective local anesthesia, the surrounding tissues are loosened and the tooth removed with forceps. Most patients tolerate this procedure well and recover quickly with standard post-care steps.
Surgical extractions are more involved and are used for roots that are curved, fused, or when the tooth is fractured at the gum line. The surgeon makes a small flap in the gum, removes minimal bone if necessary, and may divide the tooth into sections for safer removal. Because these procedures can be more invasive, we provide detailed pre- and post-operative instructions and discuss pain management strategies beforehand.
In every case we emphasize infection control, precise technique, and careful closure of the site when needed. If stitches are placed, we’ll explain whether they are dissolvable and when to return for follow-up. Clear expectations and step-by-step guidance are a core part of our approach.
Healing after an extraction follows predictable stages, and your actions in the first few days have a major influence on comfort and outcome. Immediately following the procedure you’ll be given gauze to bite on, which helps the socket form a stable blood clot. Maintain steady pressure as instructed; this clot is the foundation for healthy tissue repair and should not be disturbed.
Protect the area from mechanical irritation until numbness subsides. Avoid chewing directly on the extraction site, and be mindful of accidentally biting your lips or tongue while the local anesthetic is in effect. We’ll provide guidance on pain control and, if prescribed, antibiotics — follow any medication instructions closely to support healing.
Swelling can be expected, especially after surgical extractions. Applying ice to the cheek in short intervals during the first 24 hours helps limit inflammation. Rest, a soft-food diet for a few days, and gentle oral hygiene practices around the site all contribute to a smoother recovery.
Managing gauze and bleeding
Use the provided gauze to apply firm pressure for the first hour, replacing it as directed. Minor oozing up to 24 hours is common, but persistent heavy bleeding should prompt a call to the office.
Protect the numb area
Until the anesthetic wears off, avoid chewing or touching the area to prevent accidental injury to the lips, gums, or tongue.
Medication and infection prevention
If antibiotics are prescribed, complete the full course. For pain, take over-the-counter or prescribed medicine according to instructions and consider taking a dose before numbness fades to stay ahead of discomfort.
Protect the clot
Avoid rinsing vigorously, spitting forcefully, or using straws during the first day or two to prevent dislodging the blood clot that forms in the socket.
Control swelling with ice
Apply an ice pack to the outside of the cheek in short intervals on the day of surgery to reduce swelling and discomfort.
No smoking
Smoking and use of tobacco products significantly hinder healing and increase the risk of complications. Avoid all forms of tobacco for at least the first week after extraction.
Diet and hydration
Stick to cool, soft foods for the first 48–72 hours and avoid hot, spicy, or carbonated beverages. Keep hydrated, but sip gently.
Oral hygiene
Brush carefully and avoid the extraction site for a few days. After 24–48 hours, gentle rinses with lukewarm salt water can help keep the area clean without disturbing the clot.
Follow-up care
If stitches were placed or if the extraction was complex, we’ll schedule a follow-up visit to monitor healing and remove sutures if necessary. Keep any appointments so we can confirm recovery is on track.
If pain, swelling that worsens after the third day, persistent bleeding, or other unexpected symptoms occur, contact the practice promptly so we can assess and address the issue.
Choosing where to receive dental care is an important decision. Our team emphasizes thoughtful planning, clear communication, and gentle technique to make extractions as safe and comfortable as possible. From pre-procedure planning and imaging to careful surgical technique and follow-up, each step is designed to protect your oral health and support a smooth recovery.
We coordinate with specialists when a case requires advanced surgical care, and we collaborate with your other healthcare providers if medical conditions influence treatment decisions. When tooth replacement becomes part of the long-term plan, we can discuss options like fixed bridges, removable prosthetics, or dental implants, and help you weigh the clinical benefits of each choice.
Our focus is on delivering reliable care that respects your concerns and returns you to full function quickly. If you have questions about extractions, what to expect, or how we can support your recovery, please contact us for more information. We’re here to help you make confident, well-informed decisions about your oral health.

A tooth extraction is a clinical procedure in which a dentist removes a tooth from its socket in the jaw. Extractions may be recommended when a tooth is severely decayed, fractured beyond repair, affected by advanced periodontal disease, or when a primary tooth obstructs eruption of a permanent tooth. The goal of extraction is to stop pain or infection and to protect the health of surrounding teeth and tissues.
Decisions about removal always follow a thorough examination and diagnostic imaging when appropriate. We prioritize preserving teeth when restoration is possible, but extraction becomes the safest option when preservation would compromise oral health. Your dentist will explain the reasoning and the alternatives so you can make an informed choice about care.
Simple extractions are performed on teeth that are fully visible in the mouth and have straightforward root anatomy; these procedures are typically completed with local anesthesia and specialized forceps. Surgical extractions are used for teeth that are impacted, broken at the gum line, or have complex root structures, and they may require a small incision, removal of some bone, or sectioning of the tooth for safe removal. Both approaches aim to minimize trauma and protect adjacent structures.
Because surgical extractions are more involved, they require more detailed preoperative planning and postoperative instructions to support healing. The dentist will review imaging and explain which technique is appropriate for your situation and whether a referral to an oral surgeon is recommended. Clear expectations about the procedure and recovery help reduce anxiety and improve outcomes.
Preparation begins with a comprehensive medical and dental history review so the team can identify medications, medical conditions, or allergies that could affect treatment. You may be asked to adjust certain medications or obtain medical clearance for complex medical histories; any such guidance will come from your provider based on current clinical standards. Diagnostic imaging, such as digital radiographs, is often taken to map root shape and nearby anatomy.
On the day of the appointment, follow instructions about eating, drinking, and arriving with a responsible companion if sedation is planned. Bring a list of current medications and be prepared to discuss concerns about anesthesia or pain control so the team can select the most appropriate comfort measures. Clear communication before the procedure makes the experience more predictable and safer.
Local anesthesia is used routinely to numb the area around the tooth and is effective for most simple extractions, allowing patients to remain awake and comfortable. For patients with anxiety or for more invasive surgical extractions, additional options such as oral conscious sedation may be offered to promote relaxation while maintaining protective reflexes. In cases requiring advanced sedation or general anesthesia, the practice will coordinate care with qualified specialists when appropriate.
Your provider will review the risks and benefits of each option and tailor the approach to your medical history, anxiety level, and the complexity of the extraction. Pre-procedure instructions will vary depending on the chosen sedation method and should be followed closely to ensure safety. Always disclose prior reactions to anesthesia and any respiratory or cardiac conditions that could influence sedation choices.
Immediately after extraction you will be asked to bite on gauze to help form a stable blood clot in the socket; controlled pressure for the first hour reduces bleeding and supports healing. Mild to moderate discomfort and localized swelling are common in the first 48–72 hours and can be managed with prescribed or over-the-counter analgesics and cold therapy as recommended by your clinician. It is important to avoid disturbing the clot by not rinsing vigorously, spitting forcefully, or using straws during the initial 24–48 hours.
Eating soft, cool foods, resting, and keeping the head elevated for the first day help reduce bleeding and swelling. Follow-up instructions will include guidance on oral hygiene, activity restrictions, and signs to watch for that warrant earlier evaluation. Adhering to these directions promotes uneventful healing and reduces the risk of complications.
Protecting the blood clot that forms in the socket is essential; avoid rinsing vigorously, spitting, or using straws for the first 24–48 hours to prevent dislodgement. After the initial period, gentle rinses with lukewarm salt water can help keep the area clean without irritating healing tissues, and careful brushing of the surrounding teeth should be continued to maintain oral hygiene. If sutures were placed, your dentist will explain whether they are dissolvable and when to return for a follow-up visit.
Control swelling with intermittent ice packs during the first day and progress to warm compresses if advised for persistent stiffness after 48 hours. Stay hydrated and choose soft, nonspicy foods while avoiding items that require heavy chewing on the surgical side. Notify the practice if you experience severe or increasing pain, persistent or heavy bleeding, fever, or other concerning symptoms so the team can evaluate you promptly.
Minor bleeding, temporary swelling, and mild pain are common and typically resolve with conservative measures; persistent heavy bleeding or increasing pain may indicate the need for clinical reassessment. One specific complication, dry socket (alveolar osteitis), occurs when the clot is dislodged and the socket becomes exposed, causing intense pain a few days after extraction. If dry socket or infection is suspected, the clinician will clean the socket and may place medicated dressings and prescribe appropriate medications to control symptoms and promote healing.
Infections are managed with localized care and, when indicated, antibiotics based on clinical judgment and medical history. Nerve injury and damage to adjacent teeth are rare but possible, and preoperative imaging plus careful surgical technique reduce these risks. The practice provides clear instructions on when to return for evaluation so complications can be treated early and effectively.
Many extractions can be performed safely in a general dental office, but certain situations call for referral to an oral and maxillofacial surgeon. Complex impactions, medical conditions that increase procedural risk, or teeth with unusual root anatomy may be better managed by a specialist with advanced training and operating-room resources. Your dentist will evaluate radiographs and overall risk factors and recommend a referral when it benefits safety and outcome quality.
When a referral is recommended, the practice coordinates the transfer of records and collaborates with the specialist to ensure seamless care. The patient will be informed about what to expect from the specialist’s evaluation and postoperative plan, and the original dentist remains available to assist with follow-up and any restorative needs after healing. Clear communication between providers safeguards continuity of care.
Removing a tooth alters the local anatomy and can affect chewing, esthetics, and the position of adjacent teeth over time, so appropriate planning for replacement is often part of comprehensive care. Replacement options include fixed bridges, removable prosthetics, and dental implants; the choice depends on oral health, bone volume, adjacent tooth condition, and long-term functional goals. Your dentist will discuss clinical considerations for each option and help you understand the timing of replacement to preserve bone and alignment.
If you are a patient of Ramsi Dental, we coordinate restorative planning with your clinical needs and preferences and can refer you to specialists when implant placement or complex prosthetics are indicated. Early discussion about replacement helps guide extraction technique, socket preservation measures, and follow-up so that the final result supports both function and appearance. Maintaining regular follow-up allows the team to monitor healing and plan restorations at the appropriate time.
Contact the practice promptly if you experience severe or increasing pain after the third day, heavy or prolonged bleeding, fever, swelling that worsens instead of improving, or any foul-smelling discharge from the socket. These symptoms can indicate infection, dry socket, or other complications that need clinical assessment and possible treatment. If you have difficulty breathing, swallowing, or feel faint, seek emergency care immediately.
For routine concerns such as suture questions, mild discomfort, or clarification of post-op instructions, call during normal office hours to arrange a follow-up appointment. Timely communication with your dental team ensures problems are identified early and managed effectively so healing proceeds as expected.

We’d love to hear from you! Whether you have questions about our services, want to schedule an appointment, need guidance on your dental care, or simply want to learn more about how we can help you achieve a healthy, confident smile, our friendly and knowledgeable team is here to assist you.
Visit us at Ramsi Dental or reach out by phone or through our online form. We’re committed to making your experience easy, welcoming, and stress-free, and we’ll respond promptly to ensure you get the care you need.