A cavity begins as a tiny area of decay and, left unchecked, can weaken the structure of a tooth. A dental filling rebuilds the missing tooth material, seals the cavity against bacteria, and returns the tooth to normal chewing function. When placed correctly, a filling preserves as much healthy tooth as possible while preventing further damage.
Fillings are among the most common restorative procedures in general dentistry because they are predictable, minimally invasive, and effective. The exact steps and materials used will vary depending on the size and location of the decay, the patient’s bite, and aesthetic priorities. The goal is always the same: eliminate disease, restore shape, and protect the tooth.
Our approach emphasizes precision and comfort so that treatment is efficient and enduring. The team takes time to explain the stage of disease, the recommended restorative option, and what to expect during and after the appointment so you can make an informed decision about your care.
Humans have attempted to repair damaged teeth for millennia, using whatever materials were available. Over the last two centuries the field has moved from primitive restorations to scientifically engineered materials designed to match tooth function and appearance. Each new material addressed limitations of those that came before it: durability, seal against bacteria, biocompatibility, or cosmetic acceptability.
Modern restorative dentistry offers a broad palette of options, from long-standing metals to tooth-colored ceramics and resin-based composites. Innovations have focused on materials that bond to the tooth, conserve more natural structure, and blend seamlessly with surrounding enamel for a more natural smile.
With these advances, clinicians can tailor restorations to the needs and expectations of each patient — balancing longevity, appearance, and the condition of the remaining tooth. Proper technique and careful case selection remain as important as the material chosen.
We prioritize restorative strategies that preserve healthy tooth tissue while delivering predictable outcomes. That begins with a thorough examination and, when appropriate, digital imaging to evaluate the extent of decay and the health of adjacent teeth and tissues.
Treatment is planned around function and aesthetics. When a filling will restore both the tooth’s strength and its appearance, we discuss the available options and recommend the material that provides the best long-term result for that particular situation.
Comfort and communication are central to the experience. We use local anesthesia for routine procedures and discuss additional measures for patients who feel nervous about dental visits, aiming to make treatment as smooth and stress-free as possible for every patient we see.
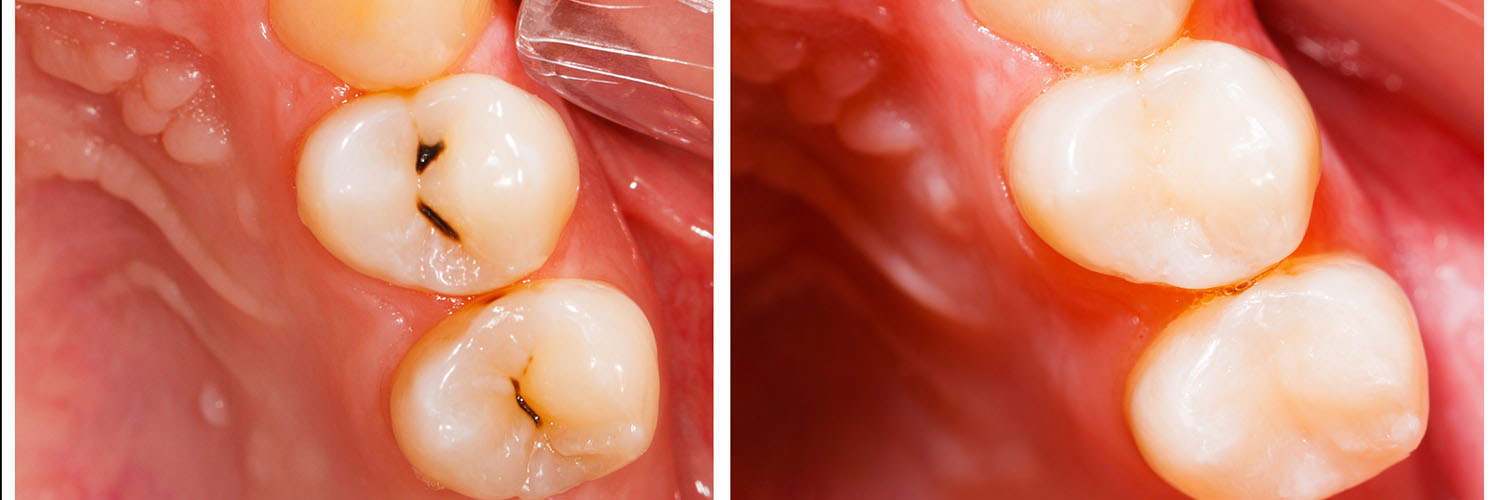
There is no single “best” filling for every situation. The ideal choice depends on the tooth’s location, the size of the defect, aesthetic goals, and how much chewing force the restored tooth must endure. Understanding the strengths and trade-offs of each material helps you and your clinician select the most appropriate option.
Conservative restorations that bond to the tooth can preserve structural integrity, whereas some materials are chosen primarily for durability in high-stress areas. When appearance matters, tooth-colored options are usually preferred; when longevity under heavy chewing forces is the main priority, other materials may be more suitable.
We’ll review the pros and cons of each option and explain why a particular material is recommended. The decision is collaborative and guided by clinical evidence and practical experience.
Composite resins are made of a durable resin matrix filled with glass or ceramic particles and are matched to the shade of your tooth. Because they bond to the remaining tooth structure, composites can allow for more conservative preparations and a tighter seal against bacteria.
They are often the first choice for front teeth and smaller to moderate cavities on chewing surfaces. While highly aesthetic, composites can be susceptible to gradual staining or wear in high-load areas and may require replacement sooner than more wear-resistant materials in some cases.
Amalgam has a long clinical history and remains a strong, wear-resistant option for large posterior restorations where appearance is less of a concern. Its physical properties make it reliable in situations that demand toughness and low maintenance over many years.
Glass ionomer materials bond chemically to tooth structure and release fluoride over time, which can be beneficial in areas at higher risk for recurrent decay. They are commonly used in baby teeth, in restorations near the gum line, or as temporary or transitional materials.
Because they are less wear-resistant than composites or ceramics, glass ionomers are usually reserved for low-stress areas or situations where their protective properties are most valuable.
Ceramic or porcelain restorations are fabricated outside the mouth and then bonded into place as inlays or onlays. These indirect restorations are highly aesthetic, resistant to staining, and very durable when properly designed and cemented.
They are often chosen for larger defects where a direct filling would compromise longevity, combining a natural appearance with excellent wear properties.
Gold remains an excellent restorative material due to its durability, biocompatibility, and stability. While less common today because of cost and aesthetics, gold can be an appropriate choice for certain large restorations where longevity and fit are prime concerns.
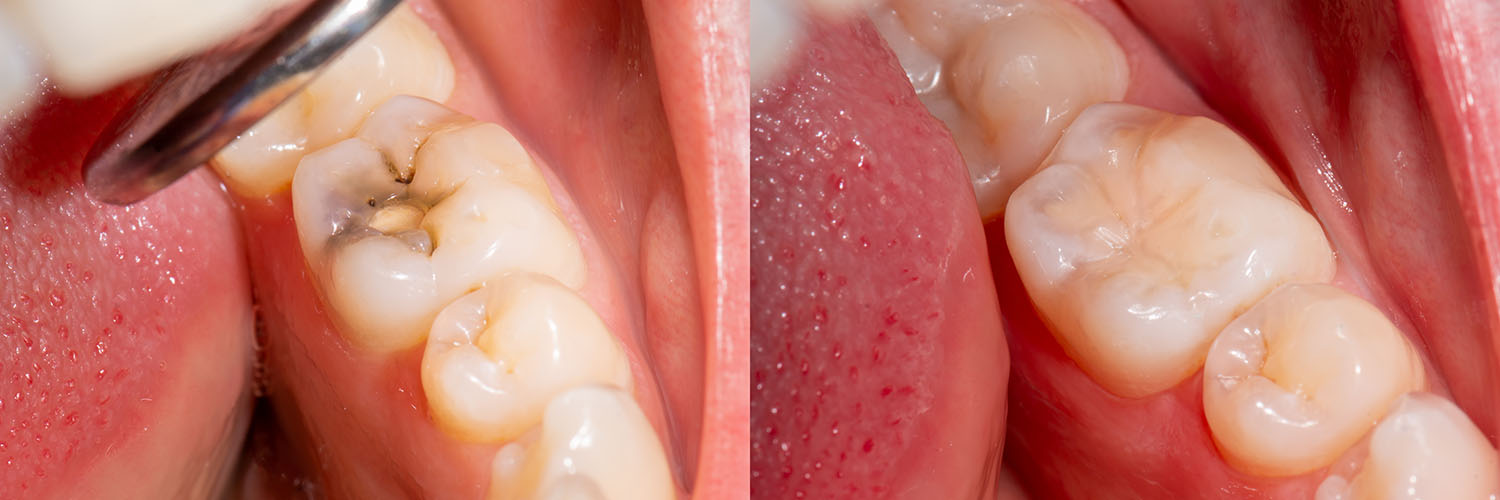
An initial evaluation determines the extent of decay and the most suitable restorative approach. Once a plan is agreed upon, treatment begins with removing the diseased tissue and preparing the tooth to receive the chosen material. This preparation preserves healthy tooth structure whenever possible.
Local anesthesia is commonly used so the procedure is comfortable; patients typically feel little to no sensation while the clinician works. Instruments such as a precision dental handpiece, air abrasion, or, in select cases, a dental laser may be used to remove decay.
Direct restorations like composites and glass ionomers are placed and shaped in the same visit, while indirect restorations such as inlays or onlays require fabrication in a dental laboratory and a separate appointment for cementation. After placement, the restoration is polished and the bite is checked and adjusted for comfort and function.
For patients who feel anxious, options for additional relaxation or sedation can be discussed. Our team aims to provide a calm, respectful experience and to keep you informed at each step of the process.
The lifespan of a filling depends on the material used, the size and location of the restoration, and how well the tooth is cared for afterward. Good daily hygiene, a balanced diet, and regular professional exams and cleanings are the most reliable ways to extend the life of any restoration.
Avoiding habits that place excessive stress on restorations—such as chewing ice, using teeth as tools, or grinding—can prevent early failure. If you have a strong bite or bruxism, night guards or other protective measures may be recommended to shield restorations from undue wear.
During routine dental visits, the clinician will assess restorations for marginal integrity, wear, and recurrent decay. Small repairs or adjustments made early can often extend the useful life of a restoration and protect the underlying tooth.
Most patients recover quickly after a filling. It is normal for a treated tooth to feel slightly different for a short period as the nerve adjusts to the work. Mild sensitivity to temperature or pressure often resolves within days to a few weeks.
If you experience worsening pain, prolonged sensitivity, swelling, or any signs of infection, contact the practice promptly. Early evaluation can determine whether a simple adjustment is needed or if additional treatment is required to address the concern.
Our clinicians will give you specific instructions after your procedure and advise when to resume normal activities, what foods to avoid briefly, and how to manage any residual numbness safely.
Protect yourself while numb
After anesthetic, avoid chewing, drinking hot liquids, or touching the area until sensation returns to prevent accidental bites or burns.
Expect small changes in how the tooth feels
It’s common for a restored tooth to feel a little different. If your bite feels uneven or you notice persistent interference, the restoration can be adjusted for comfort.
Short-term sensitivity is normal
Sensitivity to cold, hot, or sweet foods can occur but usually diminishes within a few days to weeks. If sensitivity worsens or does not improve, schedule an evaluation.
Care for the restoration
Brush twice daily, floss regularly, and keep your routine dental appointments. Proper oral hygiene and periodic check-ups help detect issues early and support the long-term success of your filling.
We take pride in providing careful, evidence-based restorative care. If you have questions after treatment or notice any concerns, please contact our office.
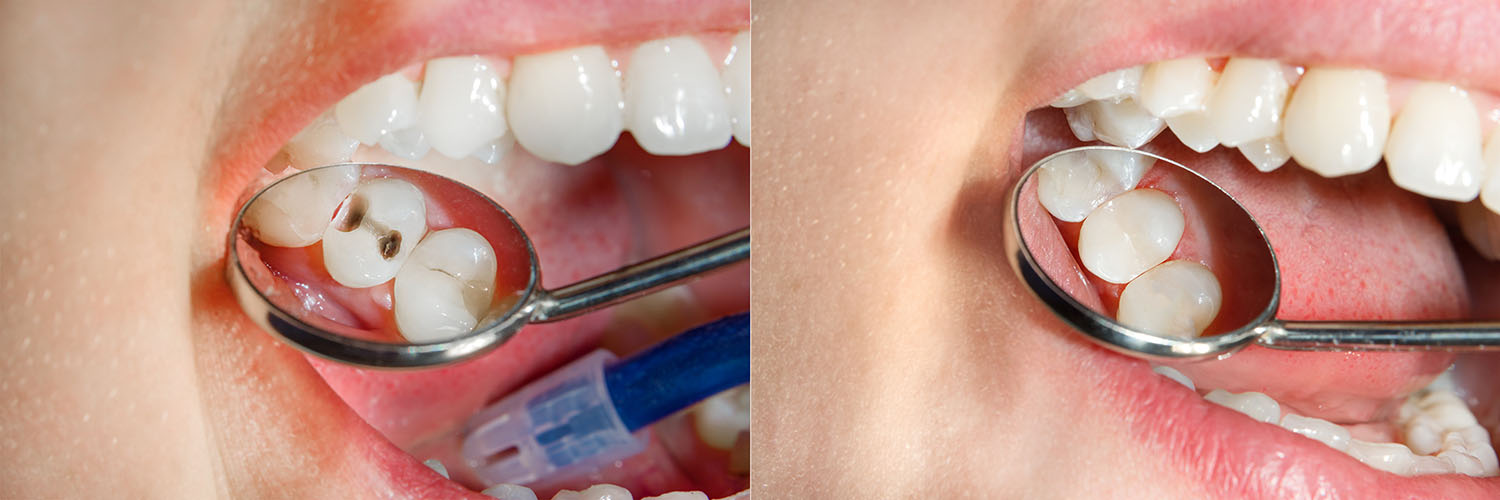
In summary, modern dental fillings are versatile solutions that stop decay, rebuild tooth form, and protect against future problems. With careful diagnosis, skillful placement, and sensible home care, restorations can preserve natural teeth for many years. Contact us for more information about how a filling might help your smile.

Dental fillings repair areas of tooth structure lost to decay or minor damage by rebuilding form and sealing the cavity. They restore a tooth's ability to withstand normal chewing forces and help prevent bacteria from reentering the lesion. When placed with careful technique, fillings preserve as much healthy tooth as possible while restoring function.
The material chosen for the filling bonds or adapts to the remaining tooth and is shaped to reestablish natural contours. Proper marginal seal and occlusal adjustment are important to avoid premature wear or discomfort. Regular follow-up lets clinicians monitor the restoration and the surrounding tooth structure over time.
Common filling materials include tooth-colored composite resin, silver amalgam, glass ionomer cement, and laboratory-made ceramics such as porcelain inlays or onlays. Composites offer strong cosmetic results and conservative preparations, while amalgam provides long-standing durability in high-stress posterior teeth. Glass ionomers release fluoride and bond chemically to dentin, making them useful in certain clinical situations.
Ceramic or porcelain inlays and onlays are fabricated outside the mouth and offer excellent aesthetics and wear resistance for larger defects. Each material involves trade-offs of longevity, wear characteristics, and appearance that clinicians weigh when recommending a restoration. The final selection is based on clinical evidence, tooth location, and the patient's functional and aesthetic priorities.
At the office of Ramsi Dental the treatment plan begins with a thorough examination and, when needed, diagnostic imaging to evaluate the size of the defect and the condition of surrounding tooth structure. The clinician then considers the tooth’s role in chewing, aesthetic concerns, and how much natural tooth remains to determine the most appropriate material. This collaborative discussion helps align clinical goals with patient preferences.
Factors such as the presence of heavy biting forces, the location of the restoration, and the desire for a seamless appearance influence the recommendation. In some cases a direct composite will be ideal, while larger defects may be better served by an indirect ceramic restoration or a durable metal option. The practice explains the pros and cons so patients can make an informed choice.
Treatment usually begins with local anesthesia to ensure comfort, followed by removal of decayed tissue and preparation of the cavity while preserving healthy tooth structure. The clinician then places the chosen material, shaping and curing or bonding it as needed to restore proper form and function. Final polishing and bite adjustment complete the procedure so the restoration feels comfortable and natural.
Direct restorations like composites or glass ionomers are often completed in a single visit, whereas indirect restorations such as inlays or onlays require a laboratory phase and a second appointment for cementation. Throughout the appointment the team will explain each step and answer questions to keep the patient informed. For anxious patients, additional supportive measures can be discussed before treatment begins.
Most patients experience little to no discomfort during the procedure because the area is numb under local anesthesia and modern techniques minimize sensitivity. It is normal to feel mild soreness or increased sensitivity for a few days as the nerve adapts to the restoration, and this typically resolves without intervention. If sensitivity worsens or persists beyond a few weeks, the tooth should be re-evaluated.
After the anesthetic wears off, avoid chewing on the treated side until normal sensation returns to prevent accidental biting. If bite interference or sharpness is noticed once sensation returns, the restoration can be adjusted quickly to restore comfort. The practice will provide specific post-procedure guidance to manage any short-term symptoms.
The lifespan of a filling varies according to the material used, the size and location of the restoration, and the patient's oral habits and hygiene. Composite restorations can last many years with good care but may show gradual wear or staining in high-load areas, while ceramics and well-placed metal restorations can provide long-term durability. Recurrent decay at restoration margins or wear from bruxism are common reasons a filling may need replacement.
Maintaining excellent oral hygiene, avoiding harmful habits like chewing ice or opening packages with teeth, and attending regular dental exams help extend the useful life of a restoration. Early detection of marginal breakdown or recurrent decay allows for less invasive repairs. When indicated, protective measures such as night guards can reduce excessive forces on restorations and prolong their serviceable life.
In the immediate weeks after treatment, continue gentle brushing and flossing while being mindful of any temporary sensitivity in the treated area. Eat softer foods for the first day if your bite feels unusual, and avoid very hard or sticky items until you are confident the restoration is functioning normally. Follow any specific instructions your clinician provides regarding analgesics or topical care.
Keep scheduled follow-up visits so the clinician can assess the restoration’s marginal integrity and your bite. If you notice persistent sensitivity, a rough feeling, or changes in how the tooth contacts its opposing tooth, arrange an evaluation promptly. Proper daily care and periodic professional maintenance are the most reliable ways to protect your restoration.
Signs that a filling may be failing include increasing or prolonged sensitivity to temperature or pressure, sharp or persistent pain, visible cracks or roughness on the restoration, and swelling or signs of infection in the surrounding gum tissue. A sudden change in bite or the feeling that a restoration is loose should prompt prompt evaluation. Dark discoloration at the margin or recurrent decay beneath a filling can compromise the tooth and necessitate repair.
Early assessment often allows for conservative solutions such as small repairs or replacement of the restoration before more extensive treatment is required. If you experience swelling, fever, or intense pain, seek immediate evaluation as these can be signs of an advancing infection. Routine dental exams play an important role in detecting developing problems before symptoms appear.
When treating children, clinicians consider the size and lifespan of the primary tooth, the child’s risk for future decay, and behavior management needs during the appointment. Materials such as glass ionomer cements may be favored in certain situations for their fluoride release and bonding properties, while direct composites are used when aesthetics and durability are suitable. Minimally invasive techniques that conserve tooth structure are prioritized to support long-term dental health.
Decay patterns, cooperation level, and preventive measures are discussed with caregivers so treatment and home care are coordinated. For anxious or very young children, behavioral techniques or appropriate sedation options can be considered to ensure a safe, positive experience. Regular preventive care and early intervention reduce the need for extensive restorations in the future.
A crown or onlay is recommended when a tooth has lost substantial structure, when a defect is too large for a durable direct filling, or when the remaining tooth would be weakened by a simple restoration. Indirect restorations such as porcelain onlays or crowns distribute chewing forces more effectively and can protect the tooth against fracture. The clinician evaluates the extent of damage, root health, and occlusal demands to determine whether a more extensive restoration is the best long-term option.
When an indirect solution is chosen, impressions or digital scans guide fabrication of a restoration that restores strength and aesthetics while conserving tooth tissue where possible. Discussing the rationale for a crown or onlay helps patients understand the trade-offs between preserving natural tooth and ensuring longevity. If you would like a personalized assessment, the team at Ramsi Dental can explain the clinical reasons for each option and the expected outcomes.

We’d love to hear from you! Whether you have questions about our services, want to schedule an appointment, need guidance on your dental care, or simply want to learn more about how we can help you achieve a healthy, confident smile, our friendly and knowledgeable team is here to assist you.
Visit us at Ramsi Dental or reach out by phone or through our online form. We’re committed to making your experience easy, welcoming, and stress-free, and we’ll respond promptly to ensure you get the care you need.