We help people restore comfort, function, and confidence after tooth loss by offering carefully planned, evidence-based restorative options. Missing teeth do more than change the way your smile looks — they alter how your bite performs, increase wear on surrounding teeth, and can set off a chain of changes in the jaw and supporting tissues. This page explains why prompt replacement matters, how modern dental bridges work, what to expect during care, and how to protect your investment for years to come.
When a tooth is lost, the immediate effect is often cosmetic, but the consequences extend deeper. Adjacent teeth can begin to tilt or drift into the empty space, changing the alignment of the bite and creating new areas that are harder to clean. Over time, these shifts can lead to uneven wear, bite discomfort, and an increased risk of cavities and gum problems where food and plaque accumulate.
Opposing teeth — those that used to meet the missing tooth when you bite — can move downward or upward into the gap, a process called extrusion. This misalignment can interfere with chewing efficiency and create an uneven distribution of force across the teeth, which accelerates wear and sometimes contributes to fractures or cracks in otherwise healthy teeth.
Bone loss in the jaw is another important concern. Teeth stimulate the bone around their roots during normal function; when a tooth is absent, the underlying bone gradually remodels and shrinks. This change in bone volume can alter facial contours and make future restorative options more complex. Replacing missing teeth in a timely, planned way helps maintain oral function and the structural foundation of the mouth.
Today’s dentistry offers a spectrum of restorations designed to meet different clinical situations and personal preferences. Fixed dental bridges provide a non-removable option that restores chewing function and fills visible gaps in a predictable fashion. Removable partial dentures are practical in some cases, while dental implants provide a root-level replacement that preserves bone and offers long-term stability.
Choosing the right solution is a collaborative process between the patient and the dental team. Factors such as the number and location of missing teeth, the health of neighboring teeth, bone quality, and the patient’s goals for appearance and function influence the recommended approach. A thorough assessment helps match the method to the individual’s anatomy and lifestyle.
The aim of every restorative plan is the same: reestablish reliable chewing, protect remaining teeth from adverse movement, and create a natural-looking smile that fits comfortably into daily life. With modern materials and laboratory techniques, restorations can be both durable and highly esthetic, blending seamlessly with natural teeth.
Traditional fixed bridges use crowns on teeth adjacent to the gap to support one or more replacement teeth, called pontics. This approach is well-suited when the neighboring teeth already require crowns or are strong enough to serve as anchors. The result is a fixed restoration that feels and functions much like natural dentition.
Cantilever bridges are a variation in which a pontic is supported from only one adjacent tooth. This design can be useful in areas with limited supporting teeth or when placing support on one side is preferable; however, it places different mechanical demands on the abutment tooth and is selected with care to avoid overloading the supporting structures.
Maryland (resin-bonded) bridges rely on metal or ceramic wings bonded to the back of adjacent teeth. They are conservative because the neighboring teeth typically need minimal or no reduction, but they are best for replacing a single front tooth where biting forces are lower. Their success depends on careful case selection and occlusion management.
Implant-supported bridges replace missing teeth without altering adjacent natural teeth. Dental implants act as artificial roots and can support one or several pontics. Because they help preserve bone and avoid placing load on neighboring teeth, implant-supported bridges are often recommended when sufficient bone is available or after appropriate bone augmentation.
A successful bridge begins with a detailed clinical evaluation. That assessment reviews the health of gums and underlying bone, the condition of neighboring teeth, bite patterns, and any history of restorative work. Dental imaging, including 2D and 3D scans when needed, helps the team visualize bone volume and tooth positions to design an appropriate solution.
Gum health is a key factor. Active periodontal disease must be controlled before placing a long-term restoration, because inflammation and bone loss undermine the foundation for crowns, bridges, and implants. The treatment plan may include scaling and root planing, improved home care routines, and targeted periodontal therapy to establish a healthy baseline.
When implants are part of the plan, the evaluation also considers systemic health, bone quality, and any medications that could affect healing. In some cases, bone grafting or sinus elevation is recommended to create a stable platform for implant placement. Treatment sequencing — such as placing implants first and allowing healing before fabricating the final bridge — is tailored to biological needs and cosmetic goals.
The process for a traditional fixed bridge typically begins with preparation of the abutment teeth, impressions to capture precise details, and placement of a temporary restoration while the laboratory fabricates the permanent prosthesis. Temporary crowns protect prepared teeth, maintain appearance, and help the team evaluate function and esthetics before final cementation.
Implant-supported restorations involve surgical placement of implants followed by a healing period that allows the implants to integrate with the bone. Depending on the clinical situation, a provisional restoration may be provided for immediate esthetics. Once integration is complete and the tissues are stable, the final bridge is fitted and adjusted for optimal bite and comfort.
During recovery, mild soreness, swelling, or sensitivity can occur but typically resolves within a few days to weeks. Follow-up visits are important to monitor healing, refine occlusion, and ensure the restoration fits comfortably. The dental team will explain any temporary restrictions, such as avoiding hard or sticky foods while healing, and provide guidance on caring for the new restoration.
Daily care is essential for the longevity of any bridge. Effective brushing and the use of interdental cleaners or special floss designed for bridges help remove plaque at the margins and below pontics. Keeping surrounding teeth and gums healthy reduces the risk of decay and periodontal disease, both of which can jeopardize a restoration.
Regular professional checkups allow the dental team to monitor the condition of the bridge and the supporting structures. Bite adjustments, replacement of worn cement, or treatment of early issues can prevent more significant problems down the road. Routine hygiene appointments also help control plaque and inflammation that are difficult to manage with home care alone.
Be attentive to changes in comfort, fit, or chewing ability. Although modern materials are durable, no restoration is indestructible. Promptly reporting looseness, unusual sensitivity, or recurring soreness lets the clinician address concerns before they affect adjacent teeth or the underlying bone.
Replacing missing teeth with a well-planned dental bridge can restore function, stabilize the bite, and preserve facial structure. If you’d like to learn more about the types of bridges available, whether a bridge is right for your situation, or what to expect from treatment, please contact us for more information. We’re happy to help you explore options and make an informed decision about restoring your smile.

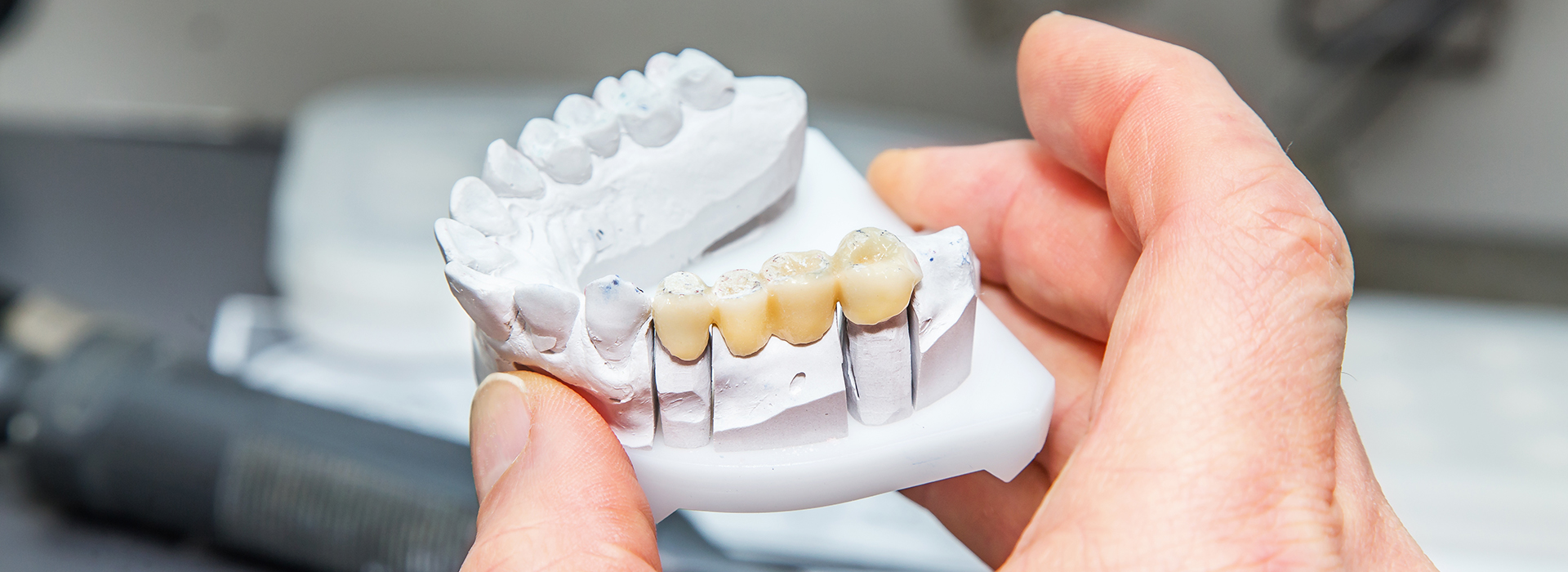
A dental bridge is a fixed restoration that replaces one or more missing teeth by spanning the gap with prosthetic teeth called pontics. Bridges are supported either by natural teeth that are fitted with crowns or by dental implants acting as artificial roots. The prosthesis restores chewing function, fills the visible space left by missing teeth, and helps maintain proper bite relationships.
Bridge components typically include abutment crowns, connectors, and pontics that are fabricated from durable materials such as porcelain fused to metal or all-ceramic systems. The restoration is designed to distribute biting forces across the supporting structures while matching the color and shape of adjacent teeth. At the office of Ramsi Dental, clinicians evaluate the anatomic and functional needs to recommend the most appropriate bridge design for each patient.
Candidates for a dental bridge generally include patients with one or more missing teeth and healthy adjacent teeth or adequate bone for implant support. The condition of the neighboring teeth, gum health, bite alignment, and overall oral hygiene habits play key roles in determining suitability. A comprehensive clinical exam and dental imaging allow the team to assess whether a fixed bridge, a resin-bonded option, or an implant-supported solution is most appropriate.
Patients with active periodontal disease or extensive decay will usually need treatment to stabilize the mouth before a long-term restoration is placed. Smoking, certain systemic conditions, and medications that affect healing are also considered during treatment planning. The goal is to select an option that preserves remaining tooth structure, restores function, and supports long-term oral health.
Traditional fixed bridges use crowns on the teeth adjacent to the gap to support one or more pontics and are commonly chosen when those abutment teeth are strong or already need crowns. Cantilever bridges attach to only one adjacent tooth and are reserved for areas with limited support or lower biting forces, but they require careful case selection due to different mechanical stresses. These designs offer a predictable, nonremovable restoration when abutment teeth can safely bear the load.
Maryland or resin-bonded bridges rely on metal or ceramic wings bonded to the backs of adjacent teeth and are often recommended for a single front tooth because they preserve more natural tooth structure. Their conservation of enamel makes them appealing when minimal preparation is preferred, but their success depends on favorable occlusion and lower anterior biting forces. Careful occlusal management helps reduce the risk of debonding in these conservative restorations.
Implant-supported bridges replace missing teeth without altering neighboring natural teeth by placing implants where roots once were and attaching pontics to those fixtures. When bone volume and medical factors permit, implant-supported options preserve jawbone, avoid loading adjacent teeth, and provide excellent long-term stability. The choice between implant and tooth-supported bridges is based on clinical findings, patient preferences, and the overall restorative plan.
Preparation begins with a thorough clinical evaluation that includes periodontal assessment, tooth and root health checks, and appropriate imaging such as panoramic or cone-beam scans when needed. The clinician will review your dental history, current restorations, and bite to ensure that any active disease is addressed and that the supporting structures are stable. Treatment sequencing may include periodontal therapy, root canal treatment, or minor restorative work to create a reliable foundation for a bridge.
If implants are part of the plan, additional preparation can include evaluating bone volume and considering grafting procedures to build adequate support. The team also discusses aesthetic goals and material choices so the laboratory can fabricate a prosthesis that matches surrounding teeth. Clear communication about expectations, healing time, and oral hygiene requirements helps patients arrive prepared for a predictable outcome.
The process for a traditional fixed bridge typically begins with preparing the abutment teeth by reshaping their surfaces to receive crowns, followed by precise impressions to capture the prepared teeth and the gap. A temporary bridge is placed to protect the prepared teeth, maintain aesthetics, and allow the patient to test function while the laboratory fabricates the final restoration. At the placement visit the dentist removes the temporary, checks the fit, adjusts occlusion and contacts, and permanently cements the final bridge.
Patients may experience mild sensitivity or soreness immediately after preparation, which usually resolves within a few days as the tissues adapt. Follow-up visits allow the clinician to refine the bite and verify that margins and contours support effective home care. Good oral hygiene and routine professional evaluations contribute to long-term success of the restoration.
An implant-supported bridge is anchored on two or more dental implants rather than on natural teeth, providing support that resembles the function of natural tooth roots. The treatment includes surgical placement of implants, a healing period for osseointegration, and subsequent attachment of a bridge that restores form and function. Because implants preserve bone and spare adjacent teeth from preparation, they are often recommended when long-term stability and structural preservation are priorities.
Compared with tooth-supported bridges, implant-supported restorations reduce the risk of weakening healthy neighboring teeth and can improve force distribution during chewing. They are particularly useful for replacing multiple adjacent teeth or when the abutment teeth are unsuitable for crowns. However, implant therapy requires adequate bone volume, a period of healing, and careful medical evaluation to ensure predictable integration.
Deciding between implant and tooth-supported solutions involves assessing bone quality, medical history, treatment timeline, and the patient’s restorative goals. In some cases bone augmentation or staged procedures are necessary to create a stable implant site. A personalized plan helps align surgical steps, prosthetic design, and maintenance expectations for the best functional and aesthetic outcome.
Common risks include decay of abutment teeth, periodontal inflammation, and loosening of the bridge due to cement failure or changes in the supporting structures. If the margins are not perfectly maintained or if oral hygiene is inadequate, bacteria can accumulate and lead to decay or bone loss around the abutments. Mechanical complications such as chipping, fracture of ceramic materials, or wear of opposing teeth can also occur over time depending on occlusion and parafunctional habits.
Proper case selection, precise laboratory work, and ongoing maintenance reduce the likelihood of complications. Early signs such as sensitivity, new mobility, or changes in bite should prompt a timely evaluation to prevent more extensive problems. The dental team monitors the restoration at regular visits and performs adjustments or repairs when needed to protect surrounding tissues and preserve function.
Daily oral hygiene is essential; brush twice a day with a fluoride toothpaste and clean under and around the pontic using floss threaders, specialized bridge floss, or interdental brushes. Removing plaque from beneath the bridge and at the margins of the crowns prevents decay and periodontal disease that can compromise the restoration. Rinsing and adjunctive tools such as a water flosser can be helpful for patients who find mechanical interdental cleaning challenging.
Regular professional cleanings and examinations allow your dental team to monitor the bridge, check occlusion, and identify early signs of wear or biological complications. Avoiding hard or excessively sticky foods during the initial healing period helps protect temporary and new restorations, and addressing habits such as teeth grinding can reduce mechanical stress. Consistent home care combined with routine dental visits is the best strategy for maintaining a bridge over the long term.
The lifespan of a dental bridge varies widely but many well-planned and well-maintained restorations last a decade or longer, with some lasting 15 years or more depending on materials and oral conditions. Factors that influence longevity include the health of the abutment teeth and gums, the design and fit of the prosthesis, the quality of laboratory fabrication, and the patient’s oral hygiene habits. Parafunctional habits, poor bite relationships, and untreated periodontal disease shorten the lifespan of any fixed restoration.
Selecting appropriate materials and a conservative design that preserves tooth structure can improve predictable outcomes. Regular maintenance visits enable the clinician to address wear, recement loose restorations, and manage biological changes before they lead to failure. When a bridge does reach the end of its serviceable life, the team evaluates replacement options that consider current oral health and restorative goals.
You should contact the dental office promptly if you notice looseness, persistent pain, swelling, increased mobility of adjacent teeth, or a change in the way your bite feels when chewing. These symptoms can indicate cement failure, decay under an abutment, periodontal issues, or mechanical damage to the restoration and benefit from timely assessment. Early intervention often allows for conservative repairs rather than more extensive treatment.
If you experience acute pain or significant swelling, seek an evaluation as soon as possible so the clinician can determine whether urgent care is required. For routine concerns such as minor sensitivity or gradual changes in fit, schedule a regular appointment to have the bridge inspected and adjusted if necessary. If you prefer, contact the team at Ramsi Dental to discuss symptoms and arrange an appropriate visit.

We’d love to hear from you! Whether you have questions about our services, want to schedule an appointment, need guidance on your dental care, or simply want to learn more about how we can help you achieve a healthy, confident smile, our friendly and knowledgeable team is here to assist you.
Visit us at Ramsi Dental or reach out by phone or through our online form. We’re committed to making your experience easy, welcoming, and stress-free, and we’ll respond promptly to ensure you get the care you need.